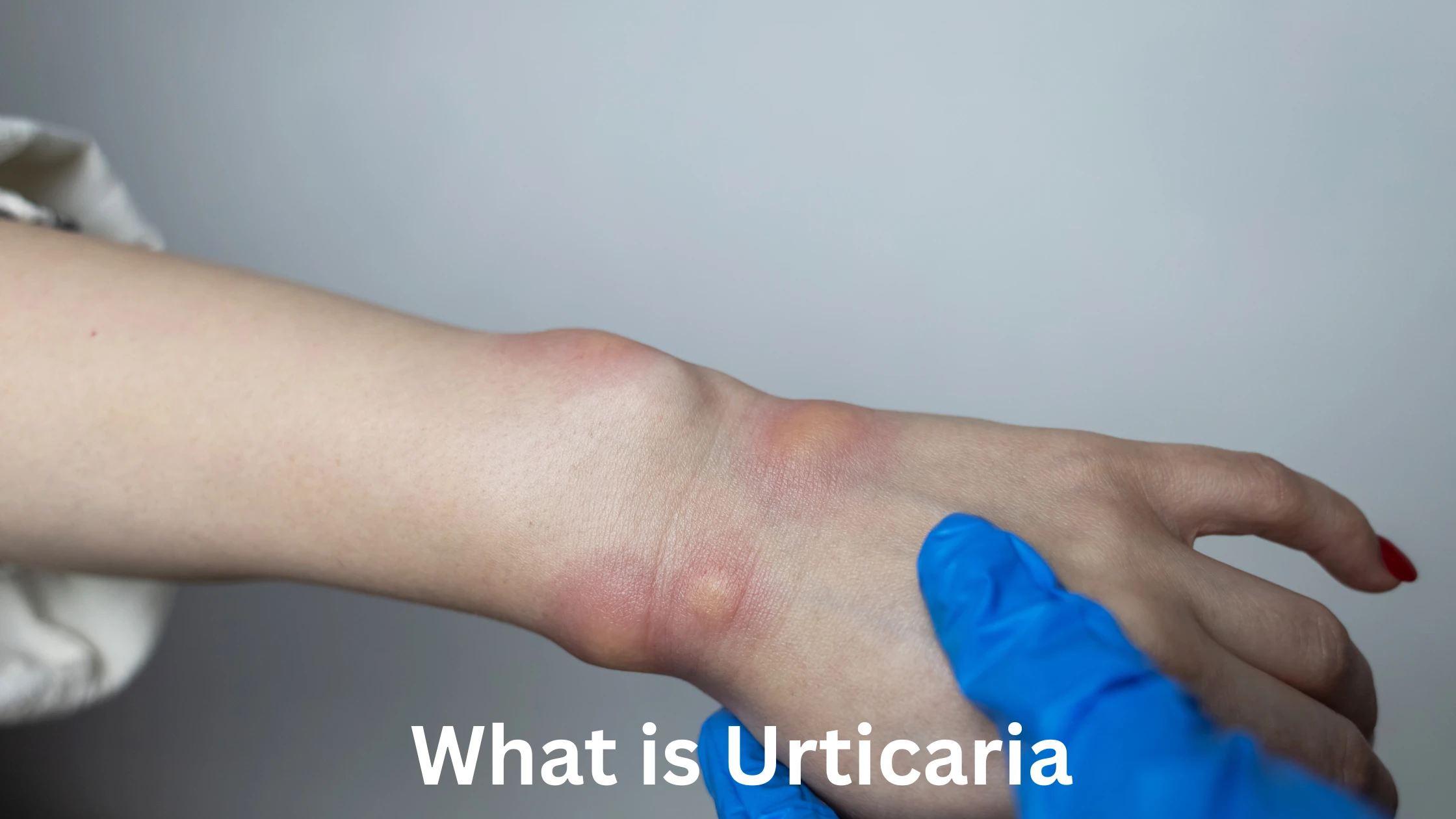
Urticaria, commonly known as hives, is a frequent skin condition that appears as red, itchy welts on the surface of the skin. These welts can vary in size—from small pinpoint spots to large patches that may merge together—and can appear suddenly, often causing discomfort and worry. Although most cases of hives are mild and short-lived, some can persist for weeks or even months, leading to frustration for those affected. Understanding the causes, symptoms, and appropriate management of urticaria can help you respond quickly and effectively if it occurs.
What Are Hives?
Hives are raised, itchy welts that appear on the skin as a result of the body’s immune system responding to a trigger. This response leads to the release of histamine and other chemicals from mast cells in the skin, which causes blood vessels to leak fluid into the surrounding tissues—resulting in the characteristic swelling and redness.
Hives can appear anywhere on the body, including the arms, legs, face, torso, and even inside the mouth or throat in severe cases. The welts often move around; one area may clear up as another becomes affected. They may also come and go over a short period, sometimes disappearing within hours only to return later.
Acute vs. Chronic Urticaria
There are two main categories of urticaria—acute and chronic—distinguished primarily by how long the symptoms last.
- Acute Urticaria: This type typically appears suddenly and lasts less than six weeks. It often results from an allergic reaction to certain foods, medications, insect stings, or infections. Common culprits include nuts, shellfish, eggs, antibiotics like penicillin, and nonsteroidal anti-inflammatory drugs (NSAIDs).
- Chronic Urticaria: If hives persist for six weeks or longer, they are considered chronic. Chronic urticaria can be frustrating because, in many cases, the exact cause remains unknown—a condition referred to as chronic idiopathic urticaria. However, in some people, chronic hives may be linked to autoimmune disorders, hormonal imbalances, or persistent infections.
Symptoms and Appearance
The hallmark symptom of urticaria is the sudden appearance of raised, itchy welts on the skin. These welts may look red or pink on lighter skin tones and may appear slightly darker or purplish on darker skin. They can vary greatly in size and shape—sometimes appearing as small dots or expanding into large patches that merge together.
Some key features include:
- Itchiness: Hives are intensely itchy and can cause significant discomfort, especially at night.
- Raised welts: The bumps are typically elevated above the skin’s surface and can feel warm to the touch.
- Changing locations: Lesions may appear in one area and then fade while new ones form elsewhere.
- Angioedema: In some cases, deeper swelling known as angioedema may occur. This affects areas like the eyelids, lips, hands, feet, or genitals. Angioedema can be painful rather than itchy and, if it involves the throat or tongue, can become life-threatening.
Common Causes of Hives
Hives can be triggered by a variety of factors. Understanding these potential causes can help in identifying and avoiding triggers.
1. Allergic Reactions
The most common cause of acute hives is an allergic reaction. Common allergens include:
- Certain foods such as shellfish, nuts, eggs, and berries
- Medications like antibiotics, aspirin, and NSAIDs
- Latex and insect stings or bites
When the immune system perceives these substances as threats, it releases histamine, leading to the appearance of hives.
2. Infections
Viral infections are another frequent cause, especially in children. Common colds, hepatitis, mononucleosis, and even certain bacterial infections can trigger hives as part of the immune response.
3. Physical Stimuli
Physical urticarias are triggered by external factors such as:
- Pressure: Tight clothing or prolonged sitting can cause pressure hives.
- Heat or cold: Temperature changes can provoke hives in sensitive individuals.
- Sunlight: A rare type called solar urticaria results from exposure to sunlight.
4. Emotional Stress
Emotional or psychological stress doesn’t directly cause hives but can exacerbate or trigger flare-ups in people who are prone to them. Stress hormones may influence immune activity, increasing histamine release.
5. Autoimmune and Idiopathic Causes
In chronic urticaria, the immune system sometimes mistakenly targets the body’s own tissues, leading to recurring hives. Autoimmune thyroid disease, lupus, and other conditions have been associated with chronic hives. However, in many cases, the cause remains idiopathic, meaning unknown.
Diagnosis
Diagnosing urticaria involves a detailed medical history and physical examination. A doctor will typically ask about:
- Duration and frequency of the hives
- Recent food intake, medications, or infections
- Any exposure to new substances or environments
In cases of chronic urticaria, blood tests, allergy testing, or thyroid function tests may be ordered to look for underlying causes.
Treatment and Management
Most cases of hives are mild and resolve on their own within hours or days. However, treatments are available to relieve symptoms and prevent recurrence.
1. Antihistamines
These are the mainstay of treatment. Non-drowsy antihistamines help block the effects of histamine and reduce itching and swelling.
2. Corticosteroids
For severe cases that don’t respond to antihistamines, short courses of corticosteroids may be prescribed to reduce inflammation.
3. Avoiding Triggers
Identifying and avoiding known triggers—such as certain foods, medications, or stressors—can significantly reduce flare-ups. Keeping a symptom diary can help pinpoint possible causes.
4. Advanced Treatments
In chronic or treatment-resistant cases, newer therapies like omalizumab (an injectable anti-IgE antibody) or cyclosporine may be used under specialist supervision.
Home Care and Lifestyle Tips
- Apply cool compresses to affected areas to soothe itching.
- Wear loose-fitting clothing made from cotton to avoid irritation.
- Avoid hot showers or baths, as heat can worsen itching.
- Reduce stress through relaxation techniques, yoga, or meditation.
- Stay hydrated and maintain a healthy diet to support skin health.
When to Seek Medical Help
While most hives are harmless, certain symptoms require immediate medical attention:
- Difficulty breathing, chest tightness, or wheezing: These could indicate anaphylaxis, a severe allergic reaction that can be life-threatening.
- Swelling of the lips, tongue, or throat: This could be a sign of angioedema, which can block airways.
- Persistent hives: If symptoms last longer than six weeks or recur frequently, consult a healthcare provider. Chronic urticaria may indicate an underlying health issue that needs evaluation.
Living with Chronic Urticaria
For those with chronic urticaria, living with daily or recurrent itching and discomfort can affect sleep, work, and overall quality of life. Support from healthcare providers, identifying triggers, and using the right medication can make a big difference. Keeping a positive mindset and managing stress effectively are also essential, as emotional well-being is closely tied to immune health.
Conclusion
Urticaria, or hives, may seem like a minor skin irritation, but it’s a clear signal from your body that something has triggered an immune response. Whether caused by allergies, infections, or unknown factors, understanding your body’s reactions is the key to effective management. For most people, hives are temporary and manageable with simple measures and antihistamines. However, if symptoms persist, become severe, or are accompanied by swelling or breathing difficulties, medical attention is crucial.
Being informed and proactive is the best way to manage urticaria—and ensure that those red, itchy welts don’t take over your comfort or peace of mind.