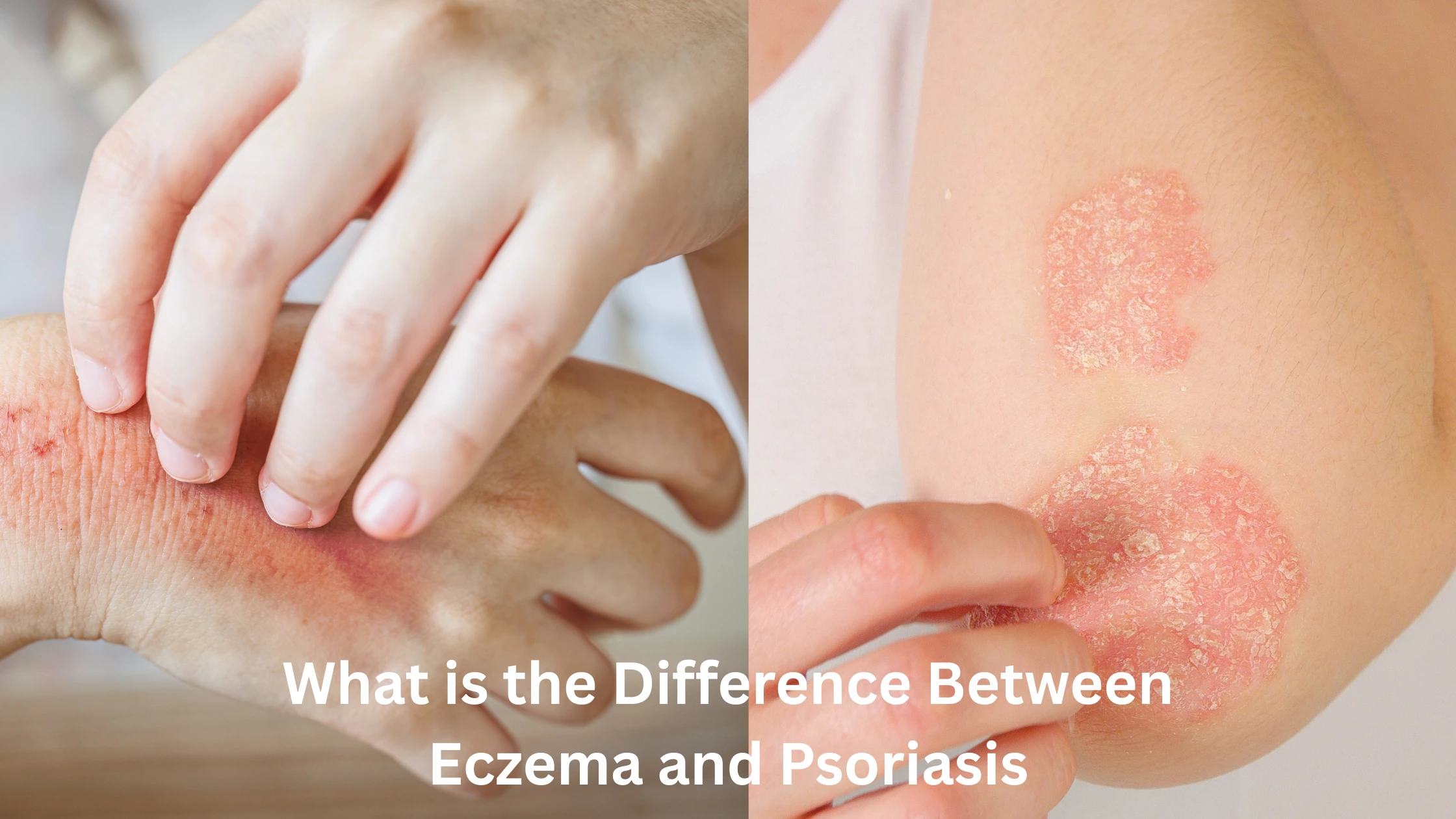
Skin conditions can sometimes be challenging to diagnose, especially when their symptoms seem similar. Eczema and psoriasis are two such conditions that are often confused, but they have distinct differences in terms of causes, symptoms, treatment options, and overall impact. In this blog, we’ll break down these two common skin disorders to help you understand how they differ and how to approach their management.
What is Eczema?
Eczema, also known as atopic dermatitis, is a chronic condition that causes inflammation, redness, and irritation of the skin. It is commonly seen in children but can also affect adults. Eczema tends to occur in areas where the skin is prone to dryness, such as the hands, feet, elbows, and behind the knees.
Causes of Eczema:
Eczema is often triggered by a combination of genetic and environmental factors, including:
- Genetic predisposition: Family history of eczema, asthma, or hay fever increases the likelihood of developing the condition.
- Environmental irritants: Such as soaps, detergents, pet dander, dust mites, and weather changes.
- Immune system response: Overactive immune responses to harmless substances can lead to inflammation in the skin.
Symptoms of Eczema:
The symptoms of eczema can vary in severity but typically include:
- Red, inflamed patches of skin
- Dry, cracked skin that may weep fluid
- Intense itching, often leading to scratching, which can worsen the condition
- Scaly, thickened skin areas
Eczema flare-ups are often cyclical, with periods of intense irritation followed by times of relief. Triggers like stress, allergens, or even certain fabrics can cause flare-ups.
Treatment for Eczema:
Managing eczema often involves:
- Moisturizers: Keeping the skin hydrated is one of the most important treatments for eczema.
- Topical corticosteroids: These help reduce inflammation during flare-ups.
- Avoiding triggers: Identifying and avoiding environmental triggers like certain soaps or fabrics.
- Antihistamines: To manage itching and discomfort.
- Immunosuppressive treatments: For severe cases, doctors may prescribe medications to suppress the immune response.
What is Psoriasis?
Psoriasis is a chronic autoimmune condition that causes skin cells to multiply at an abnormally fast rate. As a result, these cells accumulate on the surface, forming thick, scaly patches known as plaques. Psoriasis can affect any part of the body but is most commonly found on the scalp, elbows, knees, and lower back.
Causes of Psoriasis:
Psoriasis is primarily driven by immune system dysfunction, where the body’s immune cells mistakenly attack healthy skin cells. This leads to an overproduction of skin cells that cannot shed fast enough. Factors that may contribute to psoriasis include:
- Genetics: Family history plays a significant role in developing psoriasis.
- Immune system: Dysfunction in the immune system accelerates skin cell turnover.
- Environmental triggers: Stress, infections, certain medications, or skin injuries may trigger or worsen psoriasis.
Symptoms of Psoriasis:
Common symptoms of psoriasis include:
- Thick, red patches of skin covered with silvery scales: These plaques can crack and bleed.
- Itching, burning, or soreness in affected areas.
- Dry and cracked skin that may bleed.
- Nail changes: Psoriasis can also affect the nails, causing pitting, discoloration, or separation from the nail bed.
Psoriasis tends to be chronic, with flare-ups occurring intermittently, and symptoms may be aggravated by triggers like stress, skin injury, or infections.
Treatment for Psoriasis:
Psoriasis treatment is aimed at reducing inflammation and slowing the rapid growth of skin cells:
- Topical treatments: Such as corticosteroids, vitamin D analogs, and coal tar.
- Phototherapy: Using ultraviolet (UV) light to slow skin cell growth.
- Systemic medications: For moderate to severe psoriasis, oral or injectable medications that suppress the immune system may be prescribed.
- Biologics: Newer medications that target specific immune system components.
Key Differences Between Eczema and Psoriasis
While eczema and psoriasis both involve skin irritation and inflammation, they differ in several ways:
1. Cause
- Eczema is largely driven by an overactive immune response in response to environmental triggers, and genetics may play a role.
- Psoriasis, on the other hand, is an autoimmune disorder where the immune system mistakenly attacks healthy skin cells, accelerating skin cell turnover.
2. Appearance of Skin Lesions
- Eczema lesions typically appear as red, itchy, and inflamed patches of skin, which may weep fluid.
- Psoriasis presents with thick, silvery, and scaly plaques of skin, often accompanied by cracks and bleeding.
3. Location
- Eczema commonly affects the flexural areas of the body such as the elbows, knees, and behind the ears.
- Psoriasis often appears on the extensor areas such as the elbows, knees, scalp, and lower back.
4. Itching
- Eczema is associated with severe itching that can cause the skin to crack or bleed from constant scratching.
- Psoriasis can also cause itching, but it is often less intense compared to eczema.
5. Triggers
- Eczema flare-ups are usually triggered by environmental irritants, allergens, or stress.
- Psoriasis is often triggered by stress, infections, certain medications, or injuries to the skin (known as the Koebner phenomenon).
How to Differentiate and Seek Treatment
If you’re experiencing skin symptoms, it’s important to consult a healthcare professional for an accurate diagnosis. While both eczema and psoriasis are treatable, the management strategies may vary. Dermatologists often conduct skin examinations, take medical histories, and sometimes perform skin biopsies to confirm the diagnosis.
Conclusion
While eczema and psoriasis both result in uncomfortable and often unsightly skin conditions, they differ significantly in their causes, symptoms, and treatment approaches. Understanding these differences can help you seek the most effective treatments for your skin condition. Whether you’re dealing with eczema or psoriasis, early intervention and personalized care can significantly improve your quality of life. Always consult with a healthcare provider to create a treatment plan tailored to your individual needs.
If you or a loved one is struggling with eczema or psoriasis, don’t hesitate to reach out to a dermatologist to discuss the best treatment options for managing these chronic skin conditions.