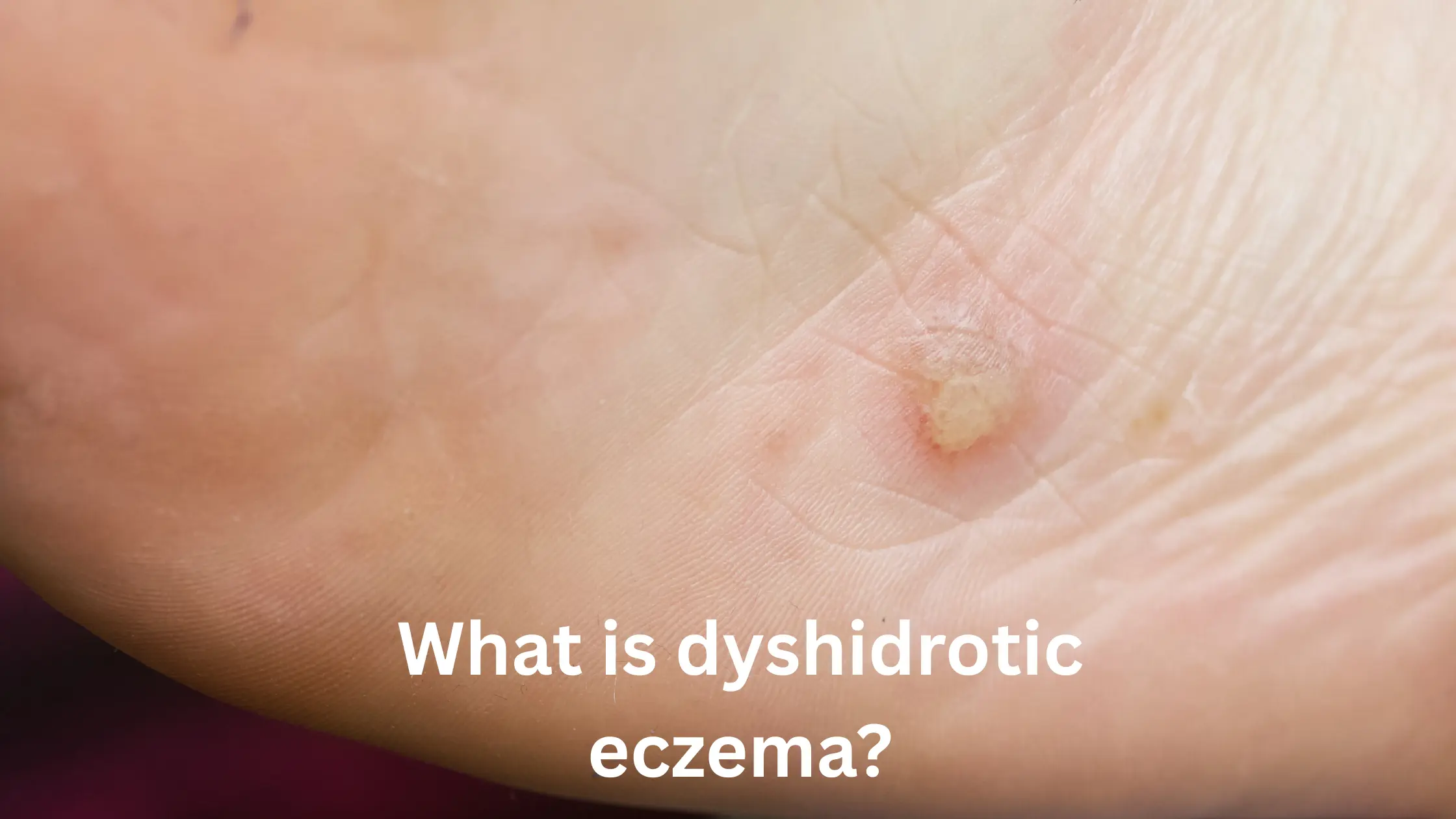
Dyshidrotic eczema, also known as pompholyx, is a type of eczema characterized by small, itchy blisters that typically form on the hands and feet, particularly on the palms and soles. This condition is often triggered by factors like stress, allergies, sweating, or exposure to certain metals like nickel. The blisters can be accompanied by redness, scaling, and a sensation of burning or stinging. Although the exact cause of dyshidrotic eczema is not fully understood, it is believed to be related to an overactive immune response. The condition can be persistent and may flare up periodically, with symptoms sometimes worsening in humid or hot conditions. Treatment often includes topical steroids, moisturizers, and antihistamines to manage symptoms, though managing triggers is also crucial in preventing flare-ups.
Dyshidrotic eczema signs and symptoms
Dyshidrotic eczema presents with several distinct signs and symptoms, which primarily affect the hands and feet. The most common features include:
- Itchy Blisters: Small, fluid-filled blisters that appear on the palms, fingers, soles, and toes. These blisters are often intensely itchy and may cause discomfort.
- Redness and Inflammation: The skin around the blisters becomes red, inflamed, and swollen.
- Cracked or Scaly Skin: As the blisters heal, the skin may become dry, cracked, and peel, leading to scaling and flaking.
- Burning or Stinging Sensation: Some individuals experience a burning or stinging feeling, especially when the blisters rupture.
- Thickened Skin: Over time, repeated flare-ups can cause the skin to thicken, with visible changes in texture.
- Blister Cluster: The blisters often appear in clusters or rows and may merge into larger areas, especially if left untreated.
The symptoms can vary in severity, and flare-ups can be triggered or worsened by stress, sweating, allergens, or exposure to irritants.
Dyshidrotic eczema causes
The exact cause of dyshidrotic eczema is not fully understood, but several factors are believed to contribute to its development. These include:
- Genetic Factors: A family history of eczema, allergies, or other skin conditions may increase the risk of developing dyshidrotic eczema. Certain genetic mutations affecting the skin barrier could make individuals more susceptible.
- Immune System Response: Dyshidrotic eczema is thought to be related to an overactive immune system. The body’s immune response triggers inflammation and an allergic reaction, causing the skin to react with blisters, itching, and redness.
- Environmental Triggers: Exposure to irritants or allergens can trigger flare-ups. Common triggers include:
- Nickel: A metal commonly found in jewelry, clothing fasteners, and even some foods.
- Detergents or Harsh Soaps: Chemicals in cleaning products or personal care items can irritate the skin.
- Moisture and Sweating: Excessive sweating, humidity, or prolonged exposure to water can contribute to flare-ups.
- Nickel: A metal commonly found in jewelry, clothing fasteners, and even some foods.
- Stress: Emotional or physical stress is a known trigger for many types of eczema, including dyshidrotic eczema. Stress can weaken the immune system, making flare-ups more likely.
- Allergic Reactions: Allergies to certain foods, pollen, or other substances can play a role in triggering dyshidrotic eczema, especially when the skin comes in contact with allergens.
- Infections: Fungal or bacterial infections may aggravate the condition or trigger new flare-ups.
- Climate: Hot, humid weather can increase the likelihood of flare-ups, while cold, dry conditions can worsen symptoms.
While these factors may contribute to the development of dyshidrotic eczema, it is important to note that each person’s experience may vary, and often a combination of these triggers is involved.
Diagnosis of Dyshidrotic Eczema
Diagnosing dyshidrotic eczema typically involves a thorough evaluation of the patient’s medical history, symptoms, and a physical examination. The key steps include:
- Medical History: A healthcare provider will ask about the patient’s symptoms, such as the location, duration, and severity of the blisters. They will also inquire about any known triggers, family history of eczema or allergies, and lifestyle factors (e.g., exposure to irritants or stress levels).
- Physical Examination: A doctor will closely examine the affected areas of the skin, looking for the characteristic small, fluid-filled blisters, redness, scaling, and cracking.
- Patch Testing: If an allergy is suspected to be a trigger, a patch test may be performed to identify specific allergens like nickel or other substances that could be causing the reaction.
- Skin Biopsy (Rarely): In rare cases where the diagnosis is unclear or when there is suspicion of another skin condition, a small sample of skin (biopsy) may be taken and analyzed in a lab.
Treatment of Dyshidrotic Eczema
While there is no cure for dyshidrotic eczema, various treatment options aim to manage symptoms, reduce flare-ups, and improve the skin’s appearance. Treatment may include:
- Topical Steroids: Prescription corticosteroid creams or ointments are commonly used to reduce inflammation, itching, and swelling during flare-ups. Stronger steroids may be prescribed for severe cases.
- Moisturizers: Regular use of thick, emollient creams or ointments helps restore the skin’s moisture barrier, preventing dryness and cracking. It’s important to apply moisturizers after washing the hands or feet to lock in hydration.
- Topical Calcineurin Inhibitors: These are non-steroid medications (like tacrolimus or pimecrolimus) that can help reduce inflammation and are often used when steroids are ineffective or unsuitable for long-term use.
- Antihistamines: Oral antihistamines may be prescribed to relieve itching and help manage allergic reactions, particularly if the eczema is triggered by allergens.
- Wet Wrap Therapy: For severe flare-ups, wet wrap therapy may be used. This involves applying a damp layer of clothing or bandages over the affected area after applying a steroid cream. The dampness helps the medication penetrate more deeply into the skin, and it helps keep the skin moisturized.
- Phototherapy (Light Therapy): In some cases, controlled exposure to ultraviolet (UV) light may be used to reduce inflammation and slow down the overactive immune response.
- Avoiding Triggers: Identifying and avoiding specific triggers—such as certain foods, metals, irritants, or stress—can help manage and prevent flare-ups. For example, avoiding nickel-containing items or wearing gloves to protect the skin from harsh detergents can be beneficial.
- Antibiotics or Antifungals (If Infected): If secondary infections occur due to the skin breaking down (such as bacterial or fungal infections), topical or oral antibiotics or antifungal medications may be prescribed.
- Stress Management: Since stress is a common trigger, relaxation techniques such as yoga, meditation, or counseling can help reduce flare-ups caused by emotional stress.
Overall, a tailored approach that combines medication, lifestyle adjustments, and trigger management is often the most effective strategy for managing dyshidrotic eczema. Regular follow-up with a healthcare provider is important to adjust the treatment plan as needed.
Dyshidrotic eczema self-care
Self-care plays an essential role in managing dyshidrotic eczema and can help reduce the frequency and severity of flare-ups. Here are some self-care tips that can help soothe the skin, prevent flare-ups, and manage symptoms:
1. Moisturize Regularly
- Use Emollient Creams: Apply thick, fragrance-free moisturizers or ointments to the affected areas several times a day, especially after washing your hands or feet. This helps keep the skin hydrated and prevents dryness and cracking.
- Avoid Harsh Soaps: Opt for gentle, fragrance-free, moisturizing cleansers instead of regular soaps that can dry out the skin.
2. Avoid Known Triggers
- Identify and Avoid Allergens: If you know certain substances trigger your eczema (like nickel, certain foods, or specific chemicals), try to avoid them. Patch testing with a dermatologist can help identify specific allergens.
- Protect Your Hands and Feet: Wear gloves when using cleaning products, handling detergents, or washing dishes to avoid irritants. Consider wearing socks to prevent friction and moisture build-up on your feet.
- Minimize Stress: Since stress is a known trigger, practice stress-reducing techniques like meditation, deep breathing, yoga, or engaging in activities that help you relax.
3. Use Cold Compresses
- Relieve Itching and Inflammation: Apply a cold compress or cool, damp cloth to the affected areas to reduce itching, swelling, and irritation.
4. Take Short, Lukewarm Showers or Baths
- Avoid Hot Water: Hot water can dry out the skin and worsen eczema. Opt for lukewarm water, and keep your showers or baths short (no longer than 10 minutes).
- Use Bath Soaks: You may try adding colloidal oatmeal to the bath, which can soothe the skin and reduce irritation.
5. Wear Loose, Breathable Clothing
- Opt for Cotton: Wear loose, soft clothing made from natural fibers like cotton to prevent irritation. Avoid tight clothing or fabrics that can trap sweat, like synthetic fibers, which can exacerbate symptoms.
6. Use Medications as Prescribed
- Follow Dermatologist’s Advice: Apply topical corticosteroids or other prescribed medications as directed by your healthcare provider. Don’t stop or reduce medication usage without consulting your doctor, as this can lead to flare-ups.
- Take Antihistamines: If itching is severe, over-the-counter antihistamines can help, but consult your doctor first to ensure they are safe for you.
7. Manage Moisture
- Keep Feet Dry: If you have eczema on your feet, be sure to dry them thoroughly after washing and change socks regularly to avoid moisture buildup, which can irritate the skin.
- Avoid Excessive Sweating: If possible, try to avoid excessive sweating or prolonged exposure to hot and humid environments, as it can worsen eczema symptoms.
8. Wear Protective Gloves When Handling Irritants
- Protect Your Skin: If you’re working with chemicals, cleaning products, or even when washing dishes, wear rubber or vinyl gloves to protect your hands from irritants.
9. Maintain a Healthy Diet
- Balance Your Nutrition: Eating a well-balanced diet rich in antioxidants and omega-3 fatty acids may help reduce inflammation and improve skin health.
- Consider Food Sensitivities: If you suspect food allergies may be contributing to flare-ups (e.g., dairy, gluten, or specific foods), consult with a healthcare provider about testing and possible elimination diets.
10. Avoid Scratching
- Relieve Itching Without Scratching: Scratching can break the skin and lead to infections. Try to resist the urge to scratch, and instead, apply a cold compress or use an anti-itch cream to alleviate the discomfort.
By following these self-care tips and working closely with your healthcare provider, you can help manage the symptoms of dyshidrotic eczema and reduce the impact it has on your daily life.