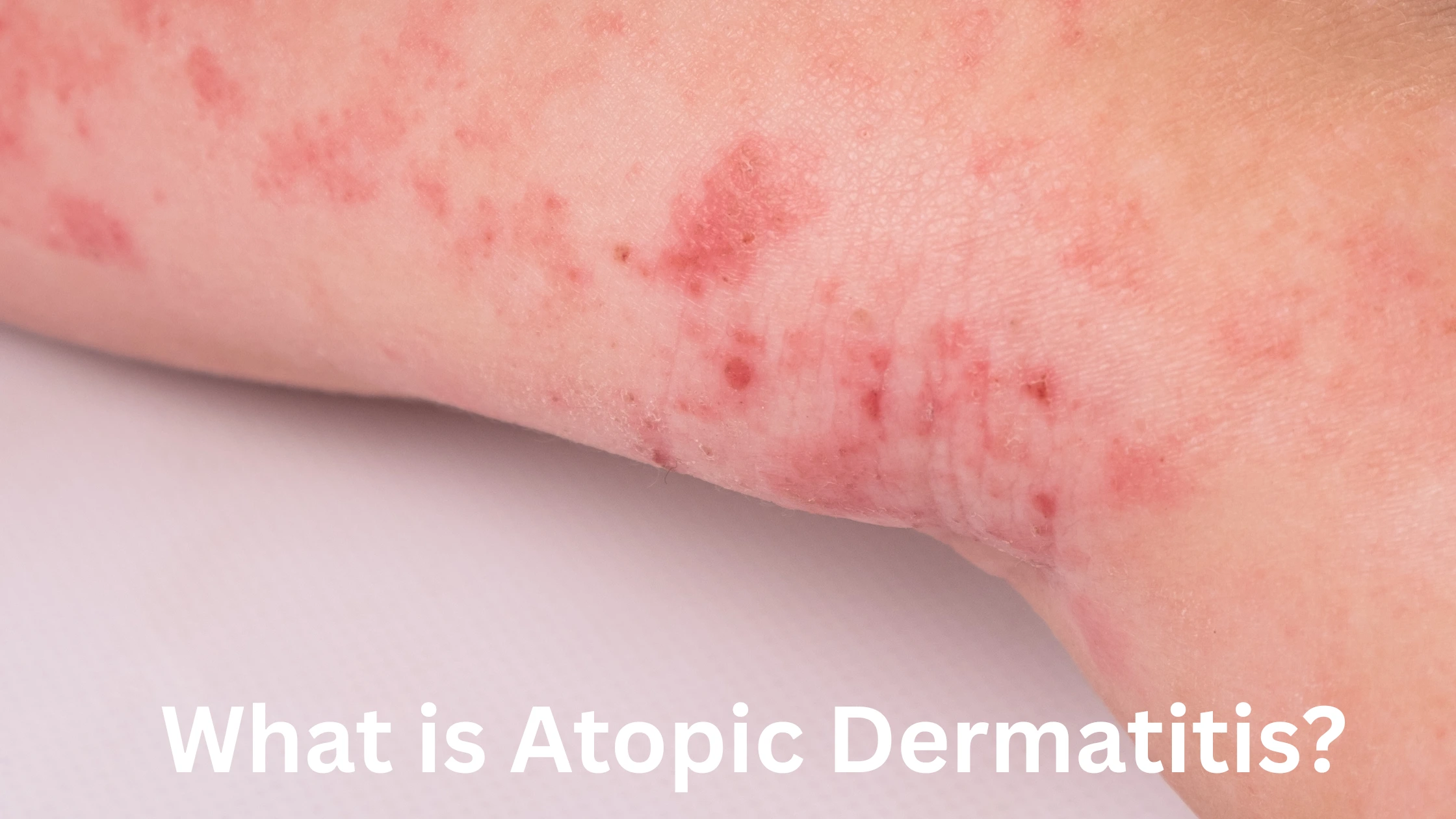
Atopic dermatitis (AD), often referred to as eczema, is a chronic inflammatory skin condition that can significantly impact one’s quality of life. It is characterized by red, itchy, and inflamed skin, often affecting areas such as the hands, feet, neck, and the inside of the elbows and knees. The condition typically begins in childhood, although it can develop at any age. Understanding its symptoms, causes, and how it’s diagnosed is crucial for managing the condition effectively.
What Does Atopic Dermatitis Look Like?
Atopic dermatitis often presents itself as patches of red, dry, and scaly skin. These patches are usually accompanied by intense itching, which can cause further irritation when scratched. In severe cases, the skin may crack, weep, or bleed, leaving it vulnerable to infection. The severity of the condition can vary, with flare-ups occurring intermittently, often triggered by environmental factors, allergens, or stress.
The appearance of atopic dermatitis differs from person to person, but it most commonly appears in the following forms:
- Dry, scaly patches: These patches often develop on the face, hands, arms, and behind the knees.
- Redness and inflammation: The affected skin becomes red, inflamed, and can be swollen.
- Thickened skin: Chronic scratching can lead to thickening and darkening of the affected areas, a phenomenon known as lichenification.
- Blisters or oozing sores: In some cases, especially during flare-ups, small blisters may form, which can break open and ooze fluid.
What Causes Atopic Dermatitis?
The exact cause of atopic dermatitis is not fully understood, but it is believed to be the result of a combination of genetic and environmental factors. Individuals with a family history of eczema, asthma, or hay fever are more likely to develop atopic dermatitis, indicating a genetic predisposition to the condition. However, several other factors contribute to the development and worsening of atopic dermatitis:
- Genetic factors: A defect in the skin barrier protein filaggrin is common in people with atopic dermatitis. This leads to a weakened skin barrier, which makes the skin more susceptible to irritants and allergens.
- Immune system dysfunction: An overactive immune system can cause inflammation in the skin, leading to the characteristic symptoms of AD. The immune system may react excessively to environmental triggers, such as pollen, dust mites, or certain foods.
- Environmental triggers: Allergens such as dust mites, pet dander, mold, and pollen can trigger or worsen flare-ups. Weather changes, particularly extreme temperatures and humidity, can also exacerbate symptoms.
- Skin irritants: Certain fabrics, soaps, detergents, and fragrances can irritate the skin and trigger flare-ups.
Symptoms of Atopic Dermatitis
The symptoms of atopic dermatitis can vary in severity and can change over time. For some people, symptoms may improve or even disappear during certain periods, while for others, symptoms persist or worsen. The primary symptoms include:
- Itching (pruritus): Itching is the hallmark symptom of atopic dermatitis and can be intense. Scratching can worsen the condition and may lead to skin infections.
- Dry, cracked skin: The skin becomes excessively dry and can crack, which makes it more susceptible to infection.
- Red or inflamed patches: These patches of red skin are often seen in areas like the face, hands, elbows, and behind the knees.
- Swelling: Inflammation in the affected areas can lead to swelling and discomfort.
- Thickened skin: Chronic scratching or rubbing can lead to thickened, leathery skin that appears darker than surrounding areas.
How is Atopic Dermatitis Diagnosed?
Diagnosing atopic dermatitis typically begins with a detailed medical history and a physical examination. Since there are no specific tests to definitively diagnose AD, the diagnosis is usually made based on the following:
- Medical history: The healthcare provider will ask about the patient’s symptoms, the frequency and duration of flare-ups, and any family history of eczema, asthma, or other allergic conditions.
- Physical examination: The doctor will examine the skin to check for the typical signs of atopic dermatitis, such as red, inflamed patches, dryness, and scaling.
- Exclusion of other conditions: Since many skin conditions can mimic the symptoms of atopic dermatitis, the doctor may need to rule out other skin disorders like psoriasis or fungal infections.
- Skin tests or blood tests: In some cases, doctors may recommend allergy testing to identify environmental or food-related triggers that may contribute to flare-ups.
While there is no single test to diagnose atopic dermatitis, the combination of a thorough history and clinical examination, along with appropriate exclusion of other conditions, allows for a conclusive diagnosis.
Managing Atopic Dermatitis
While there is no cure for atopic dermatitis, there are several treatments available to manage the symptoms and reduce flare-ups. These include:
- Topical treatments: Corticosteroid creams, calcineurin inhibitors, and other topical treatments can help reduce inflammation and relieve itching.
- Moisturizing creams and ointments: Keeping the skin hydrated is crucial in managing atopic dermatitis. Thick, emollient-rich creams can help restore the skin’s barrier function.
- Lifestyle changes: Avoiding known triggers, maintaining a regular skincare routine, and managing stress can significantly reduce flare-ups.
Conclusion
Atopic dermatitis is a common and chronic condition that requires ongoing management. By understanding its symptoms, causes, and diagnosis, individuals can take steps to reduce flare-ups and improve their quality of life. If you suspect you may have atopic dermatitis, it’s important to consult with a healthcare provider for proper diagnosis and treatment.